If you’ve been living with neck pain, you already know how much it can affect every part of your day — from turning your head to check your blind spot while driving to finding a comfortable position for sleep. You’re far from alone in this struggle. According to the Global Burden of Disease Study, neck pain affected an estimated 203 million people worldwide in 2020, and that number is projected to climb to 269 million by 2050. In the United States, neck and back pain rank among the highest healthcare expenditures, with an estimated $134.5 billion spent annually. At Barbour Orthopaedics & Spine, we understand how overwhelming it can be to navigate the wide world of treatment options, especially when the pain is affecting your ability to work, exercise, or simply enjoy life. This guide walks you through the most common cervical spine conditions, what to look for in symptoms, and the full range of treatment approaches available right here in Atlanta, Georgia.
Common Neck and Cervical Spine Conditions
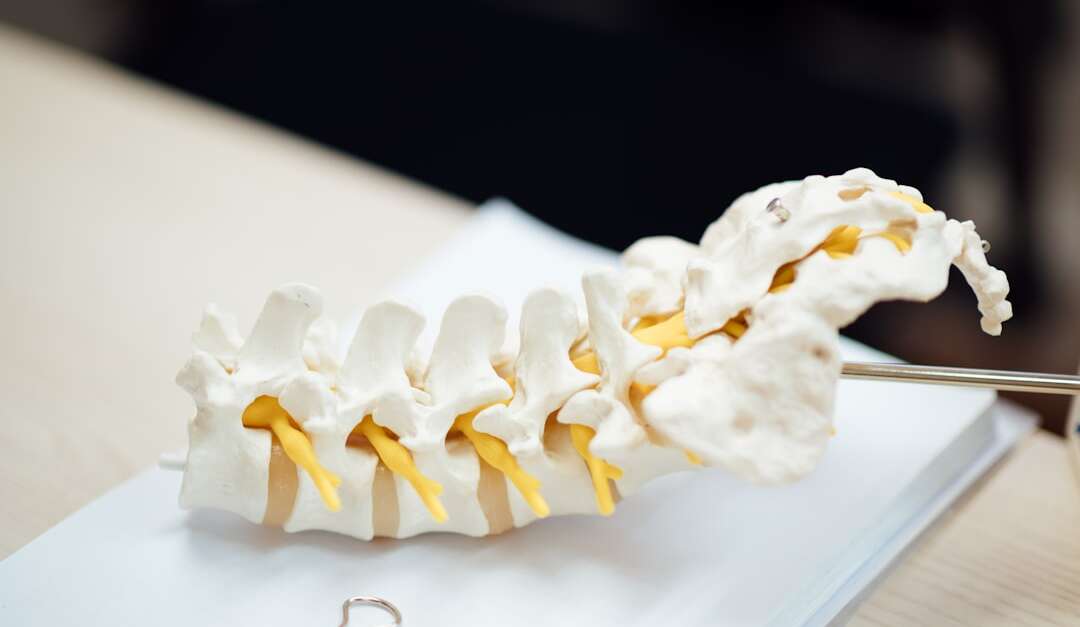
Your cervical spine — the seven vertebrae that make up the neck region from C1 to C7 — has a remarkably demanding job. It must support the weight of your head (roughly 10 to 15 pounds), allow a wide range of motion in multiple directions, and protect the spinal cord and nerve roots that control sensation and movement in your shoulders, arms, and hands. That combination of mobility and responsibility makes the cervical spine uniquely vulnerable to wear, injury, and degeneration over time.
Cervical spondylosis is one of the most prevalent conditions affecting the neck. Often called “arthritis of the neck,” it involves progressive wear-and-tear changes to the discs, joints, and ligaments of the cervical spine. These changes are a natural part of aging — spine changes often begin in your 30s, and by age 60, roughly 9 in 10 people show evidence of cervical spondylosis on imaging, even if many never experience symptoms. When symptoms do occur, they typically present as neck stiffness, aching, and reduced range of motion.
Cervical radiculopathy, commonly known as a “pinched nerve in the neck,” occurs when a nerve root in the cervical spine becomes compressed or inflamed. This can happen due to a herniated disc, bone spurs, or degenerative changes that narrow the space where nerves exit the spine. The hallmark symptoms are sharp, burning pain that radiates from the neck down into the shoulder, arm, or hand, often accompanied by numbness, tingling, or weakness. Many people find that the pain in their arm is actually more bothersome than the neck pain itself.
Cervical myelopathy is a more serious condition that develops when the spinal cord itself becomes compressed within the cervical canal. Unlike radiculopathy, which affects individual nerve roots, myelopathy can produce widespread symptoms including hand clumsiness, difficulty with fine motor tasks like buttoning a shirt, balance and gait disturbances, and a sense of heaviness or weakness in the legs. The onset is often gradual and progressive, which means it can be easy to dismiss early symptoms as simply “getting older.”
Other common cervical spine conditions include herniated discs (where the soft center of a disc pushes through its outer wall and presses on nearby structures), cervical spinal stenosis (narrowing of the spinal canal), and whiplash-associated disorders that can follow car accidents or sports injuries. Occupational factors also play a significant role — prolonged neck flexion, repetitive overhead arm work, and sustained computer use are all associated with accelerated cervical degeneration and pain.
Symptoms That Require Orthopedic Neck Care
Mild, occasional neck stiffness that resolves after a good stretch or a change in sleeping position is common and usually not a cause for concern. However, certain symptoms signal that it’s time to see a specialist. Understanding the difference between everyday stiffness and signs of a more serious cervical spine problem can help you get the right care at the right time.
You should consider seeking orthopedic neck care if you experience persistent neck pain lasting more than a few weeks that hasn’t responded to rest and over-the-counter anti-inflammatory medications. Pain that radiates from your neck into your shoulder, arm, or hand — especially if accompanied by numbness, tingling, or a “pins and needles” sensation — often indicates nerve involvement and warrants evaluation. Weakness in your grip, difficulty holding objects, or a feeling that your hand is clumsy are especially important symptoms to report, as they may suggest either radiculopathy or early myelopathy.
Gait changes deserve close attention as well. If you notice that your balance feels off, that you’re catching your toe when walking, or that your legs feel heavy or uncoordinated, these can be signs of cervical myelopathy — a condition where early intervention can make a meaningful difference in long-term outcomes. Research indicates that prognosis worsens considerably if myelopathy symptoms persist beyond 18 months without treatment, underscoring the importance of timely evaluation.
Other red-flag symptoms that warrant prompt medical attention include neck pain following trauma (such as a fall or car accident), pain accompanied by fever or unexplained weight loss, severe headaches originating at the base of the skull, and any sudden onset of neurological changes. An “electric shock” sensation that runs down your spine when you bend your neck forward is another sign that should prompt a visit to a spine specialist.
Non-Surgical Treatment Options for Neck Pain
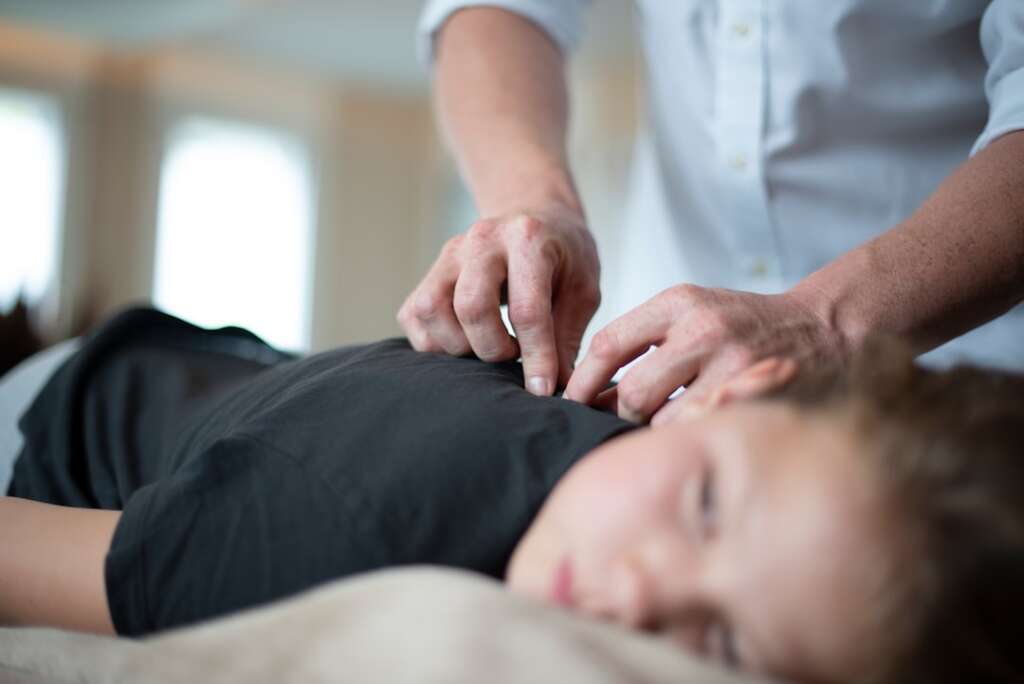
The reassuring news for most people dealing with neck pain is that the majority of cervical spine conditions respond well to conservative, non-surgical treatment. At Barbour Orthopaedics & Spine, we always explore these options thoroughly before considering surgical intervention, because our goal is to find the most effective path to relief with the least disruption to your life.
Physical therapy stands as one of the most effective and well-studied non-surgical treatments for neck pain. Research from the Bone and Joint Decade Task Force on Neck Pain found that therapies involving manual therapy and exercise are more effective than alternative strategies for patients with neck conditions. A structured physical therapy program typically focuses on strengthening the deep cervical stabilizer muscles, improving posture, restoring range of motion, and teaching you body mechanics that reduce strain on the cervical spine. Studies show that patients who complete supervised physical therapy programs experience better long-term outcomes and fewer pain recurrences compared to those who rely solely on passive treatments.
Medication management offers another layer of relief. Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and naproxen are commonly used as a first-line approach to reduce inflammation and pain. For more persistent symptoms, your physician may recommend a short course of oral corticosteroids, muscle relaxants to address associated muscle spasms, or medications specifically designed to calm nerve-related pain. The goal is always to use the lowest effective dose for the shortest necessary duration while you work on the underlying mechanical issues through therapy and lifestyle modifications.
Cervical epidural steroid injections and facet joint injections can provide targeted relief when oral medications and therapy alone aren’t sufficient. These image-guided procedures deliver anti-inflammatory medication directly to the source of pain, offering weeks to months of relief that often allows patients to participate more fully in their rehabilitation program. For certain chronic pain conditions, radiofrequency ablation — a technique that uses controlled heat to interrupt pain signals from specific nerves — can provide longer-lasting relief.
Ergonomic modifications deserve special mention, particularly for working professionals in Atlanta, Georgia who spend long hours at a desk or computer. Ensuring that your monitor is at eye level, using a headset for phone calls, and taking regular breaks to move and stretch can significantly reduce the cervical strain that contributes to chronic neck pain. A cervical collar or brace may be recommended for short-term use in some cases to support the neck during acute flare-ups.
If you’re experiencing neck pain that’s affecting your daily routine, our team at Barbour Orthopaedics & Spine can help you explore these non-surgical options and develop a personalized treatment plan. Many of our patients find significant relief without ever needing surgery.
When Neck Surgery Becomes Necessary
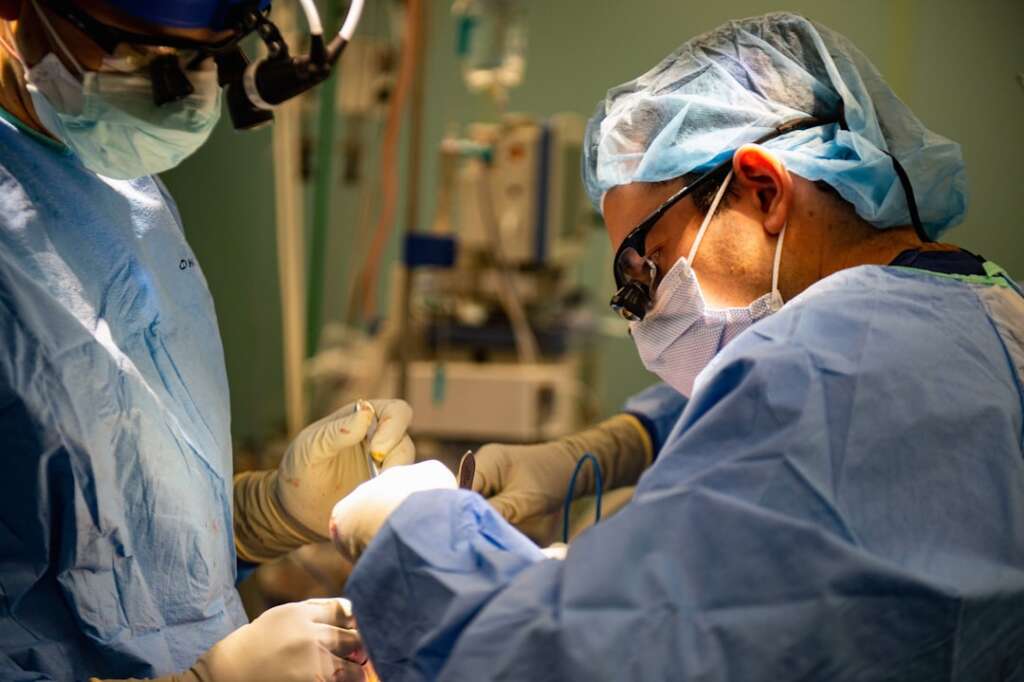
While conservative treatment works well for the majority of patients, there are situations where surgery becomes the most appropriate path forward. Surgery is typically considered when patients have failed to respond to a reasonable trial of non-surgical treatment (usually 6 to 12 weeks), when there is progressive or significant neurological compromise such as worsening weakness or coordination problems, or when spinal cord compression threatens permanent damage if left untreated.
For cervical myelopathy specifically, the 2025 AO Spine recommendations now include a conditional recommendation that surgical decompression be offered as a valid option even for mild cases, because research shows that 20% to 62% of patients with mild myelopathy may deteriorate without surgical intervention. This doesn’t mean every patient with mild myelopathy needs surgery immediately, but it highlights the importance of close monitoring and informed decision-making with your specialist.
Several surgical approaches are available for cervical spine conditions, and the right choice depends on the specific condition, its location, severity, and your individual anatomy and goals. Here’s a comparison of the most common procedures:
| Procedure | What It Involves | Best For | Recovery Timeline | Key Considerations |
|---|---|---|---|---|
| Anterior Cervical Discectomy and Fusion (ACDF) | Damaged disc removed through front of neck; vertebrae fused with bone graft and hardware | Herniated discs, bone spurs, single or multi-level disc disease | 6 to 12 weeks for initial recovery; full fusion may take 3 to 12 months | Most common cervical spine surgery; high success rates (arm pain relief in 92–100% of patients); may limit some neck flexibility |
| Artificial Cervical Disc Replacement (ADR) | Damaged disc replaced with prosthetic disc that preserves motion | Single or two-level disc disease in patients who want to maintain neck mobility | 4 to 6 weeks for initial recovery; full recovery 3 to 6 months | Preserves natural neck motion; lower risk of adjacent segment degeneration; not suitable for patients with osteoporosis or facet joint arthritis |
| Posterior Cervical Decompression and Fusion | Pressure relieved from back of neck; spine stabilized with fusion | Multi-level disease, spinal cord compression, complex cases | 8 to 12 weeks for initial recovery; several months for full healing | Used for more complex or multi-level conditions; effective for posterior compression |
| Cervical Laminoplasty | Spinal canal expanded by reshaping the lamina (without fusion) | Multi-level cervical stenosis and myelopathy | 6 to 12 weeks for initial recovery | Preserves more motion than fusion; typically used for multi-level spinal cord compression |
| Minimally Invasive Posterior Discectomy | Herniated disc material removed through smaller incisions | Select cases of disc herniation | 2 to 6 weeks for initial recovery | Less muscle damage; faster recovery; not appropriate for all types of disc problems |
It’s important to note that the decision about which surgical approach is right for you involves a thorough discussion with your spine specialist. Factors including the number of spine levels affected, the direction of nerve or cord compression, your bone quality, activity level, and personal goals all factor into the recommendation. Modern cervical spine surgery has advanced significantly, and most patients are discharged within one to two days of their procedure.
Finding the Right Neck Specialist in Atlanta, Georgia

Choosing the right specialist for your neck condition is one of the most important decisions you’ll make in your treatment journey. The cervical spine is an incredibly complex area, and outcomes are significantly influenced by the experience and approach of the treating physician.
At Barbour Orthopaedics & Spine, our approach centers on treating you as a partner in your care. We take the time to listen to your concerns, conduct a thorough evaluation, and explain your options clearly, so you can make an informed decision about your path forward with confidence.
Recovery and Rehabilitation After Neck Treatment
Whether you’ve undergone a conservative treatment program or cervical spine surgery, rehabilitation plays a central role in achieving the best possible outcome. Understanding what to expect during recovery can help reduce anxiety and set you up for success.
For patients who pursue non-surgical treatment, gradual improvement is the typical pattern. Most patients with cervical radiculopathy who respond to conservative care begin to notice meaningful improvement over 6 to 12 weeks of consistent physical therapy and activity modification. It’s important to recognize that recovery isn’t always linear — there may be days when symptoms flare — but the overall trend should be positive. Research suggests that roughly half of individuals who experience a neck pain episode will continue to have some degree of symptoms, which makes ongoing preventive strategies (strengthening exercises, good posture habits, and ergonomic awareness) essential for long-term management.
After cervical spine surgery, the recovery timeline varies based on the specific procedure. For ACDF, many patients report immediate relief of arm pain and begin returning to daily activities within a few weeks. Research shows that most patients return to driving within approximately 16 days and to work within a similar timeframe, though physically demanding jobs may require a longer recovery period. The bone fusion process itself continues for several months, during which your surgeon will provide specific guidance about activity restrictions.
For artificial disc replacement, the recovery tends to be somewhat faster because the procedure preserves motion rather than requiring bone healing for fusion. Most patients return to normal routines within four to six weeks, with full recovery occurring over three to six months. Physical therapy typically begins two to four weeks after surgery and continues for several months to help rebuild neck strength, restore range of motion, and establish healthy movement patterns.
Regardless of the treatment path, certain principles apply universally during recovery. Walking is encouraged early and often to promote circulation and prevent stiffness. Maintaining good posture, especially avoiding prolonged forward head positions while using phones or computers, helps protect the cervical spine during healing and beyond. Smoking cessation is particularly critical for surgical patients, as smoking is one of the strongest risk factors for failed bone fusion and poor healing.
Start Your Journey to Neck Pain Relief in Atlanta, Georgia
Living with neck pain doesn’t have to be your new normal. Whether you’re dealing with nagging stiffness from long hours at your desk, shooting pain down your arm that makes it hard to concentrate at work, or a progressive condition that’s starting to affect your balance and coordination, the right care can make a real difference in your quality of life.
Contact Barbour Orthopaedics & Spine today to schedule an appointment with our spine specialists. We’ll start with a thorough evaluation, take the time to listen to your concerns, and work together to create a personalized treatment plan that gets you back to doing what you love. From the latest in non-surgical therapies to advanced surgical techniques when they’re truly needed, we’re here to guide you through every step of your recovery.
Follow us on our social media!